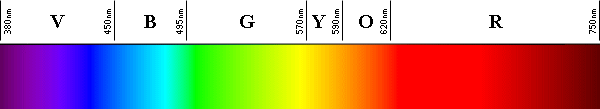
The Macula |
Anatomy, Physiology and |
Ted M. Montgomery, |
The macula lutea is the small, reddish central portion of the retina. It is about 5.5 mm in diamter and is the area providing the clearest, most distinct vision. When one looks directly at something, the light from that object forms an image on one’s macula. A healthy macula ordinarily is capable of achieving at least 20/20 (“normal”) vision or visual acuity, even if this is with a correction in glasses or contact lenses.
Not uncommonly, an eye’s best visual acuity is 20/15. In this case, that eye can perceive the same detail at 20 feet that a 20/20 eye must move up to 15 feet to see as distinctly. Some people are even capable of 20/10 acuity, which is twice as good as 20/20. Vision this sharp may be due to there being more cones per square millimeter of the macula than in the average eye, enabling that eye to distinguish much greater detail than normal.
The center of the macula is called the fovea centralis. It is about 1.5 mm in diameter and is area where all of the photoreceptors are cones; there are no rods in the fovea. The fovea is the point of sharpest, most acute visual acuity. The very center of the fovea is the “foveola,” with a diameter of only about .35 mm.
Because the fovea has no rods, small dim objects in the dark cannot be seen if one looks directly at them. For instance, to detect faint stars in the sky, one must look just to one side of them so that their light falls on a retinal area, containing numerous rods, outside of the macular zone. Rods detect dim light, as well as movement.
There are about 110,000 to 115,000 cone cells in the fovea and only about 25,000 cones in the tiny foveola. The macular/foveal area is the main portion of the retina used for color discrimination. Color vision deficiencies, which occur in less than 8% of males and in less than 1% of females, are usually hereditary, although they also can result from certain diseases, injury, or as a side effect of some medications or toxins.
The closer one’s cones are clustered together as a group, within the macula, the sharper that person’s vision, potentially, will be. Some people’s cones are “spread out” more (resulting in lesser acuity), while other people’s cones are more “clumped together” (resulting in better acuity). It is quite possible, even common, for someone to have a visual acuity better than 20/20, such as 20/15 or even 20/10 (see 20/20 compared with other acuities).
Basically, the denser the arrangement of cones is, the sharper the acuity. This is because the incoming light is falling on more of the cones, so more information about the object being viewed (and being projected as an image upon the retina) is transmitted to the brain.
The photoreceptors (rods and cones) in the retina absorb incoming light. To see any color, the retinal cone cells—most of which are located in the macula and fovea centralis—first must be stimulated by tiny photons or energy quanta of light in the visible electromagnetic spectrum.
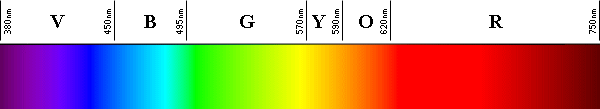
The human visual system can detect the range of light in the visible spectrum from wavelengths shorter than 380 nanometers (far violet) to longer than 750 nanometers (far red), in a vacuum or in air. Collectively, the photoreceptors in the human eye are most sensitive to wavelengths of light, in a vacuum or in air, between 530 and 555 nanometers, which is yellowish-green light.
In optical media other than a vacuum or air, such as water or glass, any color of light slows down and the wavelength shortens. What remains constant is the light’s frequency or cycles per second (that is, the number of light waves passing a given point in space per second). Thus, considering all possible media with different indices of refraction in which light can travel, the color of light is determined by its frequency.
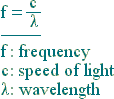 |
In the diagram to the right, the red light passes from air to glass to air. Although the wavelength changes, the frequency is constant, so the color remains the same. | 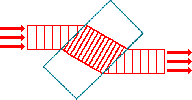 |
“Red-sensitive” cones are most stimulated by light of about
“Red-sensitive” or “L” cones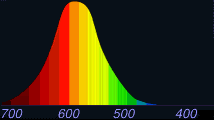 |
“Green-sensitive” or “M” cones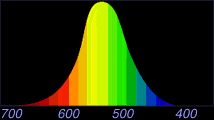 |
|
“Blue-sensitive” or “S” cones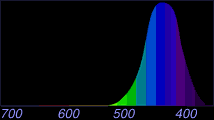 |
||
The brain must compare the input from the three different kinds of cone cells, as well as make many other comparisons. This comparison begins in the retina (which actually is an extension of the brain), where signals from “red” and “green” cones are compared by specialized red-green “opponent” cells.
These opponent cells compute the balance between red and green light coming from a particular part of the visual field. Other opponent cells then compare signals from “blue” cones with the combined signals from “red” and “green” cones. When one (or more) type of cone does not work properly, causing a color deficiency, the proper color calculations by the brain cannot take place.
If all of the cone receptors work, but one type does not work as well as the other two, an “anomalous trichromatism” results, as follows:
When one type of cone receptor does not work at all, an “anomalous dichromatism” results, as follows:
When only one type of cone receptor functions, the color deficiency is “monochromatism.” Very few people (about 3 in a million) have total “color blindness” or “achromatopsia”; they see things only in shades of white, gray and black.
Color deficiencies usually are genetic. However, sometimes such deficiencies are acquired due to retinal diseases such as glaucoma or diabetes, or by retinal poisoning by certain medications.
About 7% of males have a red-green deficiency, compared to about .4% of females. The genes for the red and green receptors (cones) are carried on the X chromosome (from the mother). As a result, a male with a defect in one of these genes does not have another X chromosome to compensate (since his other sex chromosome is Y, from his father) and, therefore, will be color deficient.
On the other hand, a female has two X chromosomes. If one X chromosome has a defective gene, her other X chromosome, as a rule, will have a compensating normal gene, enabling her to have normal color perception.
With a red-green deficiency, a person might have difficulty distinguishing between things such as red and green traffic lights or electrical wiring. Red-green color perception is altered in conditions such as optic neuritis. In some cases, a reddish “X-chrome” contact lens, worn on the non-dominant eye, can help a red-green color deficient person discern more easily between colors.
People with a less common type of deficiency cannot distinguish between blues or yellows. The gene for the blue receptor (cone) is carried on Chromosome #7. Blue-yellow color vision is diminished in many disorders, including glaucoma, diabetic retinopathy, cataract, and retinal disease.
You might wish to screen your color vision. If so, go to Color Vision Testing.
Certain conditions can affect the macula and, in turn, one’s central vision. Probably the most common is “macular degeneration,” a hereditary ocular disease. Age-related macular degeneration (ARMD) is the leading cause of irreversible blindness among Americans 65 and older.
“Dry” macular degeneration generally is caused by a thinning of the macula’s layers, and vision loss typically is gradual. However, tiny, fragile blood vessels can develop underneath the macula.
“Wet” macular degeneration can result when these blood vessels hemorrhage, and blood and other fluid further can destroy macular tissue, even causing scarring. In this case, vision loss can be rapid—over months or even weeks—as well as very devastating.
Macular tissue destroyed by either dry or wet macular degeneration cannot be repaired. In the case of the wet form, a special laser can be used to seal the leaking blood vessels in the retina. However, 1) the tiny spots where the laser burns the retina will lose vision permanently, and 2) other blood vessels may leak in the future, requiring further laser treatment.
The earliest symptom of macular degeneration usually is persistently blurred vision. As more cells of the macula are destroyed, objects become distorted (for instance, straight lines become crooked). Eventually, a small area of no vision, in the central visual field, can develop and grow in size. This can progress to the point of “doughnut” vision, where people’s faces are unrecognizable when looking directly at them, yet peripheral vision remains unaffected.
Naturally occuring carotenoids in the macula, lutein and zeaxanthin (molecular cousins of beta carotene and vitamin A), have been shown to be effective protectants against degeneration of the macula. These pigments essentially act like built-in macular “sunglasses” by absorbing, and filtering out, near-to-blue ultraviolet radiation, which potentially is the most damaging electromagnetic radiation reaching the macula.
Thus, the greater the amount of macular pigment there is, the less the risk is for developing macular degeneration. Lutein and zeaxanthin are found particularly in yellow fruits and in green leafy vegetables (especially xanthophyll-rich vegetables such as spinach, kale, collard greens, and broccoli), in eggs, and as nutritional supplements. ARMD vitamins may reduce the likelihood of progression of intermediate and advanced degrees of macular degeneration.
It is suspected that VEGF (vascular endothelial growth factor) stimulates the development and progression of neovascular ARMD. Lucentis or Avastin, both injected medications, may halt or stop the progression of ARMD.
A good way to detect early stages of macular degeneration is with an “Amsler grid.” Some cases of cystoid macular edema, central serous retinopathy, and epiretinal membrane (macular pucker) also may be detected by the Amsler grid. Two Amsler grids—one black-on-white ( ) and one white-on-black (
) and one white-on-black ( )—are shown below. Follow these instructions to use the two grids:
)—are shown below. Follow these instructions to use the two grids:


If you have not noticed problems with your vision, yet you detected broken, curved, or distorted lines (known as “metamorphopsia”) while using one or both of the above Amsler grids, it could be that you have an early stage of macular degeneration.
Try doing the Amsler grid test later today or tomorrow. If the results are repeatable, it probably would be a good idea to make an appointment to have your eyes examined by a qualified eye doctor (optometrist, optometric physician, or ophthalmologist). In any case, continue performing the Amsler grid test 2-3 times a week to monitor any changes.
Cystoid macular edema (CME) is a painless disorder affecting the macula. It is marked by the presence of multiple cyst-like (cystoid) formations which cause edema (swelling) in the macular area, resulting in blurred or decreased central vision.
Sometimes an eye with CME will be red and irritated, and a great deal of tearing may occur. Also, the eye may be tender to the touch and sensitive to light.
Although the exact cause of CME is not known, it can accompany a variety of diseases, such as retinal vein occlusion, uveitis, or diabetes. It also is present after about 3% of cataract surgeries, often many months following the surgery, even if the surgery had no complications.
If CME occurs in one eye, there is up to a 50% chance that it will appear subsequently in the other eye. Fortunately, most people recover their vision after an indeterminate period of time.
To confirm the diagnosis of CME, sometimes a test known as “fluorescein angiography” is performed. During this procedure, a fluorescent yellow dye is injected into the vein of an arm, and a series of retinal photographs are taken to show pooling of the dye in the macular area with CME (or leakage of retinal blood vessels in other conditions).
Retinal inflammation due to CME usually is treated with anti-inflammatory agents (such as Indocin or a corticosteroid) and occasionally with diuretics (such as Diamox). It may take weeks for there to be a noticeable improvement in vision.
Sometimes, the CME is caused by vitreous strands connected to and pulling on the macula, in which case a YAG laser treatment, or even a vitrectomy (removal of the vitreous), is required. Occasionally, the retinal inflammation and swelling from CME can induce a secondary glaucoma, which must be treated as a separate condition.
Central serous chorioretinopathy (CSCR), a painless condition affecting the central retina (macula or para-macular area), is caused by an accumulation of fluid under the retina, causing blurry vision, distortion of shapes, and sometimes a change in the eye’s refractive error (towards hyperopia). CSCR occurs when a small focal area of the retinal pigmented epithelium becomes compromised and allows serous fluid, from the choroidal vessels below, to leak underneath the retina, forming a sub-retinal “blister.”
The disorder affects mostly men in the age range of 20 to 50 and seems to be linked to chronic stress, whether emotional or job-related, or even with steroid use. Some experimental evidence suggests that high blood levels of epinephrine and cortisol hormones may be indirectly responsible for some occurrences of CSCR.
Most cases of CSCR will resolve spontaneously in 3-6 months. However, about 40-50% of the time, there will be recurrences of the condition. Even without a recurrence, many people have residual symptoms after the first bout of CSCR, such as visual distortion, decreased color and contrast sensitivity, and difficulty seeing at night.
Fluorescein angiography may be performed to determine the site of serous leakage, and laser photocoagulation may be used to shorten the duration of the disease condition. However, laser treatment may produce a noticeable, permanent blind spot and most likely will not decrease the chance of a recurrence.
An epiretinal membrane is scar tissue that forms over a portion of the retina. Although uncommon, it usually results from a posterior vitreous detachment. There are other names for an ERM:
With time, the scar tissue can tighten. This creates tension and traction on the retina underneath, often causing it to wrinkle or pucker. If this is in the macular area, it results in a macular pucker and sometimes macular edema. (If the macula actually tears from too much traction by the vitreous gel, a macular hole can result. However, a macular pucker will not necessarily “progress” into a macular hole.)
The deformation of the macula results in mild to severe blurriness and visual distortion. Straight lines can appear curved or wavy; this can be detected by using an Amsler grid. Usually only one eye is affected, although the other eye may be involved later in a similar way.
In many cases, the resultant blurriness and distortion of an epiretinal membrane, involving the macula, is mild enough that no treatment is necessary. Sometimes the scar tissue membrane will separate from the retina/macula and float away from the area, restoring vision.
Less frequently, the reduced vision from the macular distortion can have an adverse affect on daily activities, such as reading and driving. No eye drops, medications, nor nutritional supplements can improve the vision distorted by a macular pucker.
Instead, a vitrectomy must be performed, where the vitreous humor gel is removed. The epiretinal membrane is peeled, very carefully, away from the retina. Then a saline solution is injected to replace the vitreous gel.
Usually, following this procedure, at least half of the lost vision is restored. However, there are risks to this surgery. One possible complication, though uncommon, is retinal detachment. More commonly, a cataract may develop in that eye sooner than it otherwise would have.
Return to the Main Page ![]()
of Anatomy, Physiology & Pathology of the Human Eye
![]()
Copyright © 1998– by Ted M. Montgomery, O.D. Most rights reserved.