The retina is the innermost layer of the eye (the tunica intima or internal tunic) and is comparable to the film inside of a camera. It is composed of nerve tissue which senses the light entering the eye.
This complex system of nerves sends impulses through the optic nerve back to the brain, which translates these messages into images that we see. That is, we ôseeö with our brains; our eyes merely collect the information to do so.
The retina is composed of 10 layers, from the outside (nearest the blood vessel enriched choroid) to the inside (nearest the gelatinous vitreous humor):
- pigmented epithelium,
- photoreceptors; bacillary layer (outer and inner segments of cone and rod photoreceptors),
- external (outer) limiting membrane,
- outer nuclear (cell bodies of cones and rods),
- outer plexiform (cone and rod axons, horizontal cell dendrites, bipolar dendrites),
- inner nuclear (nuclei of horizontal cells, bipolar cells, amacrine cells, and MŘller cells),
- inner plexiform (axons of bipolar cells and amacrine cells, dendrites of ganglion cells),
- ganglion cells (nuclei of ganglion cells and displaced amacrine cells),
- nerve fiber layer (axons from ganglion cells traversing the retina to leave the eye at the optic disc), and
- internal limiting membrane (separates the retina from the vitreous).
Beneath the pigmented epithelium of the retina are these 4 layers, from the outside (furthest from the retina) to the inside (closest to the retina):
- sclera (white part of the eye),
- large choroidal blood vessels,
- choriocapilaris, and
- Bruchĺs membrane (separates the pigmented epithelium of the retina from the choroid).
Light entering the eye is converged first by the cornea, then by the crystalline lens. This focusing system is so powerful that the light rays intersect at a point just behind the lens (inside the vitreous humor) and diverge from that point back to the retina.
This diverging light passes through 9 (clear) layers of the retina and, ideally, is brought into focus in an upside-down image on the first (outermost) retinal layer (pigmented epithelium). Then, amazingly, the image is reflected back onto the adjacent second layer, where the rods and cones are located.
photoreceptors (cones and rods)
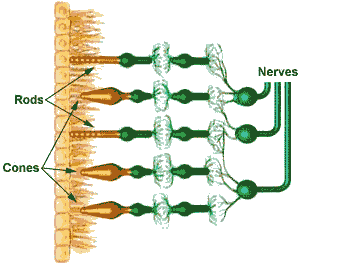 Cones and rods actually face away from incoming light, which passes by these photoreceptors before being reflected back into them. Light causes a chemical reaction with photopigments: ôiodopsinö in cones (activated in photopic or bright conditions) and ôrhodopsinö in rods (activated in scotopic or dark conditions). This begins the visual process.
Cones and rods actually face away from incoming light, which passes by these photoreceptors before being reflected back into them. Light causes a chemical reaction with photopigments: ôiodopsinö in cones (activated in photopic or bright conditions) and ôrhodopsinö in rods (activated in scotopic or dark conditions). This begins the visual process.
Activated photoreceptors stimulate bipolar cells, which in turn stimulate ganglion cells. The impulses continue into the axons of the ganglion cells, through the optic nerve, and to the visual center at the back of the brain, where the image is perceived as right-side up. (See more on the visual pathway for greater detail.) The brain actually can detect one photon of light (the smallest packet of energy available) being absorbed by a photoreceptor.
There are about 6.5 to 7 million cones in each eye. They process bright light and color and are responsible for color vision. The highest concentration of cones is in the macula. The fovea centralis, at the center of the macula, contains only cones and no rods.
There are 3 types of cone pigments. Each one is most sensitive to a certain wavelength of light in a vacuum or in air: short or ôSö about 420ľ440 nm, medium or ôMö about 534ľ545 nm, and long or ôLö about 564ľ580 nm. (A ônanometeröŚnmŚis one billionth of a meter or one millionth of a millimeter.) Once a cone pigment is bleached by light, it takes about 6 minutes to regenerate.
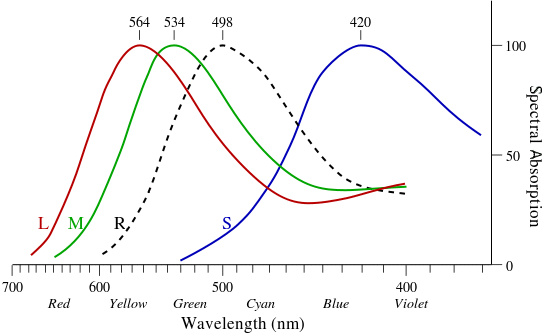
There are about 120 to 130 million rods in each retina; and they are sensitive to dim light, to movement, and to shapes. The highest concentration of rods is in the peripheral retina, decreasing in density up to the macula.
Rods do not detect color, which is the main reason it is difficult to tell the color of an object at night or in the dark. The rod pigment or ôRö is most sensitive to a wavelength of about 498 nm. Once a rod pigment is bleached by light, it takes about 30 minutes to regenerate. Defective or damaged cones result in a color deficiency; whereas, defective or damaged rods result in problems seeing in the dark and at night.
A third photopigment, melanopsin, is found in photosensitive ganglion cells in the inner retina. These cells seem to be involved in the pupillary light reflex, in the regulation of circadian rhythms, and in other non-visual and non-image forming photoresponses.
retinal detachment (RD)
Normally, with age, the vitreous gel collapses and detaches from the retinaŚan event known as a posterior vitreous detachment. Occasionally, however, the vitreous membrane pulls on and creates a tear in the retina. Vitreous fluid can seep into or beneath the retina, detaching it from the pigmented epithelium underneath.
When a retinal detachment occurs, a shower of floaters may be observed by the person experiencing the detachment. These are thousands of blood cells being liberated from a tiny blood vessel which has been broken due to the retinal tear or detachment. Sometimes the floaters are described as being like a ôshower of pepperö before the eyes.
Sudden flashes of light, as well as a ôwebö or ôveilö in front or else in the periphery of the eye, also may appear in conjunction with the onset of floaters. The retinal tear and subsequent detachment must be repaired as soon as possible, usually with one of these procedures:
- sealing it using an argon laser (ôphotocoagulationö),
- freezing it (ôcryotherapyö or ôcryopexyö),
- securing it, after cryotherapy, with a tiny belt around the equator of the eye (ôscleral buckleö surgery),
- injecting a gas bubble into the eye (in conjunction with photocoagulation or cryopexy) so that the bubble rests against the hole or tear (ôpneumatic retinopexyö), requiring the person to keep his/her head in the same position for several days, or
- removing the vitreous gel and filling the eye with a gas bubble or silicon oil (ôvitrectomyö).
If the tear and detachment are not repaired, permanent vision loss can result. The worst vision loss occurs if the macula becomes detached.
retinitis pigmentosa (RP)
One of the most devastating conditions affecting the rods is ôretinitis pigmentosa,ö an inherited disorder in which the rods gradually degenerate. With time, night vision is severely affected. Eventually, all peripheral vision will continue to be destroyed, to the point where only central or ôtunnelö vision remains.
There is no known treatment. However, since blue and ultraviolet light may make aggravate the condition, amber-colored glasses with an ultraviolet absorption coating, worn during the day, may slow down the disease process.
Studies have shown that retinitis pigmentosa is caused by mutations in the rhodopsin gene, the peripherin gene, and possibly in other genes within the rod. Mutations in the peripherin gene also may be the cause of another devastating retinal disorder: ômacular dystrophy.ö
Return to the Main Page 
of Anatomy, Physiology & Pathology of the Human Eye
Copyright ę 1998ľ by Ted M. Montgomery, O.D. Most rights reserved.
 Cones and rods actually face away from incoming light, which passes by these photoreceptors before being reflected back into them. Light causes a chemical reaction with photopigments: ôiodopsinö in cones (activated in photopic or bright conditions) and ôrhodopsinö in rods (activated in scotopic or dark conditions). This begins the visual process.
Cones and rods actually face away from incoming light, which passes by these photoreceptors before being reflected back into them. Light causes a chemical reaction with photopigments: ôiodopsinö in cones (activated in photopic or bright conditions) and ôrhodopsinö in rods (activated in scotopic or dark conditions). This begins the visual process.