 This causes the entire lens to flatten or to become less convex, enabling the lens to focus light from the far-away object.
This causes the entire lens to flatten or to become less convex, enabling the lens to focus light from the far-away object.The Crystalline Lens |
Anatomy, Physiology and |
Ted M. Montgomery, |
The transparent crystalline lens of the eye is located immediately behind the iris. It is composed of fibers that come from epithelial (hormone-producing) cells. In fact, the cytoplasm of these cells makes up the transparent substance of the lens.
The crystalline lens is composed of 4 layers, from the surface to the center:
The lens capsule is a clear, membrane-like structure that is quite elastic, a quality that keeps it under constant tension. As a result, the lens naturally tends towards a rounder or more globular configuration, a shape it must assume for the eye to focus at a near distance.
Slender but very strong suspensory ligaments, also known as zonules or zonules of Zinn, attach at one end to the lens capsule and at the other end to the ciliary processes of the circular ciliary body, around the inside of the eye. These thin ligaments or zonules hold the lens in place.
The ciliary body is circular, and the ciliary muscle within it is a sphincter muscle, shaped like a tiny doughnut. The inside diameter of the muscle gets smaller when it contracts and larger when it relaxes.
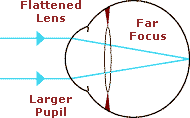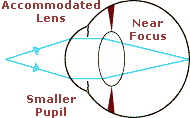
When the eye is viewing an object at a far distance (such that parallel rays of light are entering the eye), the ciliary muscle within the ciliary body relaxes. The ciliary processes pull on the suspensory ligaments (or zonules), which in turn pull on the lens capsule around its equator.  This causes the entire lens to flatten or to become less convex, enabling the lens to focus light from the far-away object.
This causes the entire lens to flatten or to become less convex, enabling the lens to focus light from the far-away object.
Conversely, when the eye views an object at a near distance, an “accommodative demand” is created. As a result, the ciliary muscle works or contracts, causing tension to be released on the suspensory ligaments and, subsequently, on the lens capsule. This causes both (front and back) lens surfaces to become more convex and the eye to be able to focus at near. (View another graphic: Accommodation of the Crystalline Lens.)
This adjustment in lens shape, to focus at various distances, is referred to as “accommodation” or the “accommodative process” and is associated with a concurrent constriction (decrease in size) of the pupil. The animated diagram above illustrates the change in stance of the ciliary body, crystalline lens, and pupil as the eye looks back and forth between far and near.
The “amplitude of accommodation” of an eye is the maximum amount that the eye’s crystalline lens can accommodate (change shape), in diopters (D). This amount is very high when a person is young and decreases with age.
The amplitude of accommodation is equivalent to the inverse (reciprocal) of the distance (“nearpoint of accommodation”) at which the emmetropic eye can focus clearly. (“Emmetropia” refers to an eye having no refractive error—no hyperopia, myopia, nor astigmatism—or it can refer to the optical system of an eye corrected to “plano” [0.00 diopters of refractive error] with glasses, contact lenses, or refractive surgery.)
| Age | Amplitude of Accommodation | Nearpoint of Accommodation (in an Emmetropic Eye) |
|---|---|---|
| 5 | 16.00 diopters | 6.3 cm (2.5 in) |
| 10 | 14.00 diopters | 7.1 cm (2.8 in) |
| 15 | 12.00 diopters | 8.3 cm (3.3 in) |
| 20 | 10.00 diopters | 10.0 cm (3.9 in) |
| 25 | 8.50 diopters | 11.8 cm (4.6 in) |
| 30 | 7.00 diopters | 14.3 cm (5.6 in) |
| 35 | 5.50 diopters | 18.2 cm (7.2 in) |
| 40 | 4.50 diopters | 22.2 cm (8.7 in) |
| 45 | 3.50 diopters | 28.6 cm (11.2 in) |
| 50 | 2.50 diopters | 40.0 cm (15.7 in) |
| 55 | 1.75 diopters | 57.0 cm (22.5 in) |
| 60 | 1.00 diopter | 100.0 cm (39.4 in) |
| 65 | 0.50 diopter | 200.0 cm (78.8 in) |
| 70 | 0.25 diopter | 400.0 cm (157.5 in) |
| 75 | 0.12 diopter | optical infinity |
Normally, the accommodative process, or accommodation, of the crystalline lens is smooth and effortless. When one changes one’s focus from far to near, the ciliary muscle quickly contracts, causing the crystalline lens to accommodate (become thicker) and the object at a near distance to become clear. Then, when looking back again at a far distance, the ciliary muscle immediately relaxes, causing the crystalline lens to revert to a thin shape and one’s far-distance vision to become clear again.
Sometimes, though, the eyes can undergo significant stress after having done several weeks or months of prolonged near work, such as reading, writing, drafting, playing video games, viewing a computer screen or a smart phone, and/or texting. Often, someone who always has had good far distance vision gradually, or even suddenly, notices that his/her far vision is beginning to blur. Often, one eye will experience a change first; then, with time, the other eye will follow. A person in this situation most likely is a victim of “nearpoint stress,” which eventually can manifest itself in myopia (nearsightedness) and/or astigmatism, resulting in blurred distance vision.
Although nearpoint stress is more common in students, from elementary school through college, it can occur at any age in the eyes of somebody performing extended periods of near work. This especially can be the case when there are not adequate breaks to rest the eyes. Sometimes, simple visual therapy techniques for convergence insufficiency or convergence excess can relieve some of the stress on the eyes (see Simple Visual Therapy).
Strained eyes can develop symptoms of asthenopia, which include eye discomfort and tiredness, headaches, and even eyelid twitching. Another symptom may be noticed when looking up from a long period of close work, and this is that objects across the room are a little blurry. The blurriness may last for a few seconds or for several minutes. In the initial stages, far away objects will clear up gradually, as the ciliary muscles slowly relax.
However, with maintained nearpoint stress over time, far distance vision can remain blurry, because the ciliary muscles are unable to relax completely. Myopia and/or astigmatism will have begun to become “embedded” within the accommodative system of the
Some people are more genetically pre-disposed to nearpoint stress, and the mechanics of nearpoint-stress-induced myopia vary from person to person. In most cases, though, the intraocular ciliary muscle controlling the eye’s crystalline lens goes into a spasm (known as “ciliary spasm”). At first, this can be temporary.
With time, though, if the stress is not relieved, this can become more permanent. It can cause the crystalline lens of the eye to take on and lock into a more curved, thicker shape (from front to back). If this takes place equally in all meridians, myopia can result; if the process is unequally distributed, astigmatism can result. This is not in conjunction with a weakening of the ciliary muscle but, rather, with a continual overaction of this muscle that controls the crystalline lens.
The full process of nearpoint stress is not completely understood. It may be that too much near work, without giving the eyes frequent and sufficient breaks to view things across the room or further away, may result in an “over-heating” of the ciliary muscle of the eye. This excess heat may be transmitted into the vitreous humor and, over time, may cause pockets of this gel-like substance to soften. Immobile organic debris (known as “floaters”), located in some areas of the vitreous and which have been there since the time of fetal development, then may begin to move around, although this may not occur for everyone.
If these particles migrate toward the center of the vitreous, they can cast shadows on the retina, resulting in the impression of “spots” or “dots” before the eyes. Floaters tend to be more prevalent in people with high myopia. However, floaters can be observed by people whose eyes have not undergone nearpoint stress and are not myopic.
Another consequence of prolonged near work can be a spasming of the ciliary muscle, which in turn can cause a constant, overly-convex shaping of the crystalline lens. This can cause images to focus in front of the retina when viewing distant objects, which is myopia.
Often, rather than both eyes being overworked an equal amount, one eye (usually the person’s dominant eye) will tend to perform a disproportionate amount of the near work. This can result, only or mostly in that eye, in the onset or progression of myopia or astigmatism. Both eyes may experience nearpoint stress changes, but the amount in the dominate eye is likely to be greater. To some extent, this refractive difference in the eyes, if great enough, also can hinder one’s depth perception to some extent.
A thorough ocular examination by a qualified, knowledgeable eye doctor usually can detect even the slightest degree of nearpoint stress in an eye. The doctor may suspect nearpoint stress when a comparison with previous measurements refractive error (especially within the past year or so) indicates a change toward myopia or astigmatism in one or both eyes.
The primary means of preventing nearpoint stress should be to reduce or eliminate the strain on the ciliary muscles of the eyes during long periods of close work. First and foremost, it is extremely important to keep near objects as far away as possible from the eyes when viewing them for more than a few minutes at a time. Good lighting on a page and proper brightness on a computer monitor/screen can be an essential key in providing good contrast, thus making text clear enough to help motivate a person to maintain the proper viewing distance.
The closer an object is to the eyes, the more effort the ciliary muscles must exert for the eyes to focus clearly on that object. Accordingly, this produces more strain on the intraocular muscles and, often, headaches. Thus, it is imperative to do these things:
Reading and writing material should be kept at least 20 inches away from the eyes, and a computer monitor should be no closer than 25 inches away—the further, the better. Occasionally, a glare-free screen can be helpful in reducing ocular discomfort; however, viewing a regular screen at a comfortable distance is more beneficial than decreasing screen glare when trying to minimize nearpoint stress.
Usually, simply looking up across the room or out of a window frequently, for a few seconds every few minutes, should relax the ciliary muscles sufficiently to prevent nearpoint stress. When looking up and away, if distant objects are blurry, this is a sign that nearpoint stress has been occurring.
One should not resume a near task at least until one’s far vision has become clear. Sometimes looking alternately from far to near and then to far again, back and forth a few times, will enhance the flexibility of the ciliary muscles and decrease the chance of a cilary spasm.
Commonly, minus lenses are prescribed for a person with myopia, even in the initial stages, enabling him/her to see clearly far away. However, when these glasses are worn to do near work, they increase the amount of nearpoint stress, since the eyes already have attempted to adapt to a near distance without the glasses. Thus, if the person wears the new glasses (which focus the eyes at a far distance) while doing all near work, it actually can accelerate the progression of the myopia.
If eyestrain, eyelid twitching, headaches, and/or temporary distance blur frequently are noticed after near work, it may be that a pair of “reading” glasses, prescribed by a qualified eye doctor—even prior to the onset of presbyopia—will be helpful in preventing or reversing myopia induced by nearpoint stress. Another option is bifocals, where the top portion of each lens contains the far prescription and the bottom portion the near prescription.
The idea behind a reading prescription of convex (plus) lenses, in either single vision glasses or in bifocals while performing near visual tasks, is that the light entering entering the eyes will be refocused by the lenses. That is, the lenses do a small amount of the focusing for the person’s crystalline lenses, reducing some or even all of the ongoing stress on the ciliary muscles. For example, the demand of print being read at 20 inches on the accomodative system of an eye (with no refractive error) is about +2.00 D (diopters). If +0.50 D glasses are prescribed, the eye needs to provide only +1.50 D of the work—that is, only 75%, rather than 100%, of the workload.
In most cases, the relief of tension on the focusing system, via the use of the proper plus lens prescription for near work, is enough to prevent over-contraction of these intraocular muscles and, thus, avert a nearpoint-stress event. A regimen of simple visual therapy techniques, in particular for convergence excess, sometimes can be used to reverse the effects (including low myopia and/or astigmatism) of the nearpoint stress.
Prevention or reversal of nearpoint-stress-induced myopia and/or astigmatism, though, is much more likely to take place very soon after the onset of the condition, rather than at a later point. If the myopic and/or astigmatic refractive error has been embedded too deeply into the eyes’ focusing systems, it can be very difficult, or impossible, to reverse.
It has been theorized that in some cases of nearpoint stress, the cornea of the eye takes on a “steeper” (more convex) shape in one or more meridians, due to prolonged pressure behind it. If indeed this occurs, the pressure may be due to frequent anterior-to-posterior expanding of the eye’s crystalline lens from focusing too much at near, inducing a compression of the aqueous fluid anterior to the lens and, thus, resulting in pressure on the posterior cornea.
In many cases, rigid gas permeable (RGP) contact lenses can retard or stop the progression of myopia and/or astigmatism. This may be evidence that a change in corneal shape can be a factor in some types of nearpoint stress. Apparently, in such cases, the rigid lens prevents the anterior cornea from becoming more convex, thus arresting the advancement of myopia in the eye.
If the aforementioned pressure on the cornea can occur from nearpoint stress, similar pressure, theoretically, could occur behind the crystalline lens of the eye, being transmitted through the vitreous gel and then to the retina. If so, it may be, in some cases, that the retina and the back of the eye (the sclera) gradually are pushed posteriorly, eventually resulting in a lengthening of the eyeball and in the onset or increase of myopia.
After age 40 in most people (both males and females), and by age 45 in virtually all, a clear, comfortable focus at a near distance becomes more difficult with eyes which see clearly (whether with or without glasses) at a far distance. This normal condition is known as “presbyopia,” and it is due primarily to a hardening and lessening of flexibility of the crystalline lens. To a much lesser extent, another factor is a generalized weakening of the ciliary muscle, which causes the lens to accommodate (change focus).
By the time one reaches age 65 or so, the crystalline lens is virtually incapable of changing shape. Unless one is nearsighted by a certain amount, it is not possible to focus objects (such as print on a page) clearly even at an arm’s length distance.
Interestingly, the first symptom of presbyopia often is not blurred print or eyestrain while reading. Rather, one may observe that objects across the room appear momentarily blurry after looking away from a near distance (that is, after reading, writing, or viewing a computer screen for awhile). This is because the crystalline lenses within the eyes have become less flexible than they used to be, resulting in their being less able to accommodate (change focus) from near to far.
With time, it will take longer and longer to refocus objects far away after having done close work. Nearpoint stress can intensify and accentuate this process.
Eventually, if presbyopic eyes are forced to continue to focus unwillingly at near, one’s far vision will become and remain noticeably blurry. For a person who never had to wear glasses to see clearly far away, myopia (nearsightedness) and/or astigmatism will have set in, requiring a far-distance prescription in glasses or contact lenses to see clearly again. For a person who already is myopic, the degree of nearsightedness will have increased, requiring a stronger lens prescription to regain clear distance vision.
A myopic (nearsighted) person with presbyopia often can remove his/her glasses to focus clearly at near. If this is too inconvenient, he/she can obtain multifocal or progressive addition lenses to be able to focus clearly at far and near with the same pair of glasses.
When a person wearing single-vision contact lenses develops presbyopia, it will be necessary to wear some type of reading prescription (in glasses) over the contacts to achieve and maintain a clear, unstrained focus at near. In many cases, bifocal or aspheric contact lenses can provide adequate vision at far and near distances, without the use of glasses.
For some people, one eye (usually the dominant eye) may be fit with a contact lens focusing that eye for far away viewing and the other eye fit with a lens focusing that eye for near viewing. This is called a “monovision” fit. However, with this arrangement, one’s depth perception (which is important when driving) may be compromised to some extent, although usually not significantly.
Note that “presbyopia” is not the same as “hyperopia” or farsightedness. Presbyopia is an age-related condition, resulting in difficulty keeping a clear, comfortable focus at a near distance, even with an eye which is not hyperopic (farsighted). On the other hand, hyperopia is a refractive error which makes it more difficult than normal to maintain a focus at a near distance than at a far away distance at any age (although, if one has a moderate to high degree of hyperopia, even maintaining a clear focus far away is difficult).
A hyperopic (farsighted) person with presbyopia generally must acquire reading glasses for near work, or else multifocal or progressive addition lenses for full-time wear. In some cases, a “monovision” contact lens arrangement also may be appropriate for a hyperopic person with presbyopia.
For some people with presbyopia, store-bought (non-prescription) reading glasses may be an option. However, store-bought glasses have equal strengths in the right and left lenses. Since most people’s eyes have at least slightly unequal refractive errors, the focusing between their two eyes will not be balanced when wearing non-prescription readers. Thus, one or both eyes may experience eyestrain. Headaches also may result.
The amount of presbyopia inevitably increases with age. Therefore, the additional “plus power” of the lens strength required to maintain a clear, unstrained focus at near will need to be increased every few years to compensate for the irreversible effect of the presbyopia. The wearing of reading glasses for presbyopia does not cause one’s near vision without the glasses to get worse. Presbyopia increases as one ages, regardless of whether or not glasses are worn for near tasks.
Normally, all the layers of the crystalline lens are clear, and light passes through it unobstructed. However, with age or due to certain systemic diseases, as well as with a cumulative absorption of ultraviolet radiation over many years, the lens material can become cloudy, yellow, brown, and even opaque. Anything in the lens which obstructs entering light is referred to as a “cataract.”
More than 50% of people over the age of 60 have some form of cataracts. It has been said that if one lives long enough, he/she will develop a cataract. Even some infants are born with a “congenital” cataract which, if left untreated, can cause permanent visual impairment or blindness, even if the cataract is removed years later.
It is not possible to remove a primary cataract without irreparably damaging the crystalline lens within which the cataract is contained. Cataract surgery involves removing most or all of the lens of the eye and replacing it with an artificial “intraocular lens” (IOL) or “lens implant,” made of a hard plastic (polymethyl methacrylate or PMMA), silicone, acrylic, or hydrogel material.
An “extracapsular” cataract extraction (ECCE) is the routine type of cataract removal. In an ECCE procedure, an opening is made in the front of the lens capsule. Through this opening, the lens nucleus is removed, either as a whole or by dissolving it into tiny pieces with an ultrasound instrument and vacuuming out the pieces, a procedure called “phacoemulsification.” In some cases, a femtosecond laser may be used to fragment the cataract into tiny segments. Next, the lens cortex also is sucked out, leaving the lens capsule in place, and into the lens capsule is inserted the artificial lens implant.
Prior to the 1980’s, the entire crystalline lens was removed in a cataract surgery, called an “intracapsular” cataract extraction (ICCE). Usually, this was performed using “cryoextraction,” where a cryoprobe froze the entire lens, permitting its complete removal. Now, in the unusual case of an intracapsular lens extraction, or ICCE, the implant lens is placed in front of the iris, rather than behind it, because there is no lens capsule to hold the implant in place. Rarely is this procedure done anymore.
Approximately 1-2% of post-cataract extraction patients develop swelling in the area of the retina responsible for central vision (the macula). This swelling occurs in cystoid spaces, and is referred to as cystoid macular edema. After an initial improvement following surgery, these patients subsequently will describe blurred vision. Cystoid macular edema can occur as early as days, or as late as several years, following surgery. Treatment options include observation, topical therapy, periocular injections, and surgery.
Naturally occuring carotenoids in the crystalline lens—lutein and zeaxanthin (molecular cousins of beta carotene and vitamin A)—have been shown to reduce the risk of cataracts. These pigments act as antioxidants within the lens, inhibiting the formation of free radicals, which can damage lenticular material and contribute to the development of cataracts.
Thus, it may be that the greater the amount of antioxidants such as lutein and zeaxanthin in the system, the less the risk of cataract formation. These two antioxidants are found particularly in yellow fruits and in green leafy vegetables (especially xanthophyll-rich vegetables such as spinach, kale, collard greens, and broccoli), in eggs, and as nutritional supplements.
Not uncommonly, following an “extracapsular” cataract extraction (ECCE), a few cells of the crystalline lens cortex remain adhered to the inner surface of the posterior lens capsule. After a few weeks or months, these cells can become opaque, resulting in a secondary cataract. Fortunately, the eye does not have to be reopened for this simple cataract to be removed.
Rather, a YAG (yttrium aluminum garnet) laser is used, in a procedure taking only a few minutes, to fire through the clear cornea and pupil and to obliterate the secondary cataract (and a small portion of the capsule behind it). This is known as a YAG capsulotomy, which enables light to pass into the eye again, unobstructed. If this laser procedure is successful, a cataract never again should pose a problem for that eye.
Return to the Main Page ![]()
of Anatomy, Physiology & Pathology of the Human Eye
![]()
Copyright © 1998– by Ted M. Montgomery, O.D. Most rights reserved.