The iris, visible through the clear cornea as the colored disc inside of the eye, is a thin diaphragm composed mostly of connective tissue and smooth muscle fibers. It is situated between the cornea and the crystalline lens. The color(s), texture, and patterns of each person’s iris are as unique as a fingerprint.
The iris is composed of 3 layers, from the front to the back:
- endothelium,
- stroma, and
- epithelium.
The iris divides the anterior compartment, the space separating the cornea and the lens, into 2 chambers:
- the larger anterior chamber (between the cornea and the iris), and
- the smaller posterior chamber (between the iris and the lens).
eye color
 The color of the iris, established genetically, is determined by the amount of pigment present in the iris structure. No pigment at all (in the case of an albino) results in a pink iris. Some pigment causes the iris to appear blue. Increasing amounts of iris pigment produce green, hazel, and brown irises (or irides).
The color of the iris, established genetically, is determined by the amount of pigment present in the iris structure. No pigment at all (in the case of an albino) results in a pink iris. Some pigment causes the iris to appear blue. Increasing amounts of iris pigment produce green, hazel, and brown irises (or irides).
There actually are two pigments, melanin and lipochrome, which determine eye color. Melanin (brown) deposition is controlled by a gene on chromosome 15. Lipochrome (yellowish-brown) deposition is controlled by a gene on chromosome 19.
Rarely, one iris can be a different color than the other iris. This is known as “heterochromia irides” and is determined genetically. Also, a section of one iris may be a different color from the rest of that iris; this is known as “heterochromia iridum” or “sectoral heterochromia iridis.” Usually, if one of these conditions is present, it is noticeable at birth, although various ocular pathologies can cause any of these conditions to be present.
From 10% to 15% of the Caucasian population will have a change in eye color with age. Sometimes, especially if the color changes in only one eye, this can be due to conditions such as Horner’s Syndrome, pigmentary glaucoma, Fuch’s heterochromic iridocyclitis, and pigment dispersion syndrome.
Iris color may appear to change temporarily, depending upon the color of clothing a person is wearing on a particular day. However, this presumed color change does not actually take place; it is a misperception by the observer, often due to variations in lighting.
pupil
In the middle of a normal iris is the pupil. It is an opening that, typically, is circular and is comparable to the aperture of a camera. The pupil helps regulate the amount of light passing through to the retina, which is at the back of the eye.
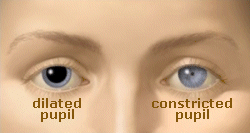 As the amount of light entering the eye diminishes (such as in a dark room or at night), the iris dilator muscle (which runs radially through the iris like spokes on a wheel) pulls away from the center, causing the pupil to “dilate.” This allows more light to reach the retina. When too much light is entering the eye, the iris sphincter muscle (which encircles the pupil) pulls toward the center, causing the pupil to “constrict” and allowing less light to reach the retina. Certain eye drops also can dilate or constrict the pupils.
As the amount of light entering the eye diminishes (such as in a dark room or at night), the iris dilator muscle (which runs radially through the iris like spokes on a wheel) pulls away from the center, causing the pupil to “dilate.” This allows more light to reach the retina. When too much light is entering the eye, the iris sphincter muscle (which encircles the pupil) pulls toward the center, causing the pupil to “constrict” and allowing less light to reach the retina. Certain eye drops also can dilate or constrict the pupils.
Constriction of the pupil also occurs when the crystalline lens accommodates (changes focus) so that the eye can view something at a near distance. This reaction is known as the “near reflex.” A representation of parasympathetic pathways in the pupillary light reflex can be seen here: parasympathetic response. Sometimes the pupil does not react properly, due to cranial nerve or muscle problems (see Pupillary Defects and Conditions Affecting the Face).
Watching television in a dark room gives some people eye aches or headaches. This is because as the brightness of the television screen fluctuates considerably every few seconds. This causes the dilator and sphincter iris muscles controlling the pupil to have to work overtime, constantly adjusting the ever-changing levels of light entering the eye.
Therefore, it is recommended that a uniform background light source is present in the room while watching television. This will cause the pupils to be slightly constricted, thus causing less variance in the size of the pupil as the television illumination changes. As a result, the muscles controlling the pupil size should become less tired.
uvea
The iris is the most anterior portion of the uvea or uveal tract (also known as the tunica vasculosa or vascular tunic). Other structures, posterior to the iris, also are part of the uveal tract. Thus, the uvea is composed of the following:
iritis/uveitis/chorioretinitis
It is not uncommon for the iris, the entire uvea, and/or the choroid/retina complex to become inflammed. Here are types of inflammation of the uveal tract:
- iritis: inflammation of the iris alone,
- iridocyclitis: inflammation of the iris and ciliary body,
- choroiditis: inflammation of the choroid alone,
- chorioretinitis: inflammation of the choroid and retina, and
- uveitis: inflammation of the entire uveal tract
Although the exact cause of an iritis or uveitis often is unknown, in many cases the inflammation is related to a disease or infection in another part of the body (that is, a systemic problem). Sometimes these (and other) diseases can cause uveal inflammation: arthritis, tuberculosis, syphilis, ankylosing spondylitis, Reiter’s syndrome, toxoplasmosis, histoplasmosis, cytomegalovirus (CMV), sarcoidosis, and toxocariasis. Infection of some parts of the body (tonsils, sinus, kidney, gallbladder, and teeth) also can cause inflammation of the iris or of the entire uveal tract.
The symptoms of iritis usually appear suddenly and develop rapidly over a few hours or days. Iritis commonly causes pain, tearing, light sensitivity, and blurred vision. A red eye, usually with inflammed blood vessels around the limbus (the junction of the cornea and sclera), often is present when there is an iritis. Some people may see floaters, which appear as small specks or dots moving in the field of vision. In addition, the pupil may become smaller in the eye affected by iritis.
Caught in the early stages, an iritis or uveitis usually is readily treated with corticosteroids and/or antibiotics. However, without treatment, or with chronic occurrences of the inflammation, there can be a permanent decrease in vision or, in rare cases, even blindness.
A case of iritis usually lasts 6 to 8 weeks. During this time, a person should be observed carefully (by an optometric physician or ophthalmologist) to monitor potential side effects from medications and any complications which may occur. Cataracts, glaucoma, corneal changes, and secondary inflammation of the retina may develop as a result of iritis and/or the medications used to treat the disorder.
malignant melanoma
A melanoma is cancer that forms in melanocytes, the cells that produce melanin. Melanin is a pigment responsible for skin color and eye color. A nevus, containing normal malanocytes, should be watched carefully, as it may develop into a malignant melanoma.
Most commonly formed on the skin, a malignant meloma also can be found within the eye, in the uveal tract, most commonly in the choroid, but sometimes in the iris. Less commonly, a melanoma can form on the conjunctiva. Increased exposure to ultra-violet radiation in sunlight often is a factor in melanoma formation in the skin and iris, but probably not in the choroid.
A choroidal melanoma, forming just beneath the retina, usually pushes up the retina. It can spread extensively throughout the choroid. The biggest concern is that the malignant cells will metastisize (spread) to other areas of the body and cause cancerous tumors elsewhere.
Large tumors, especially if they are near the optic nerve, are the most likely to metastasize. An adverse affect on vision, as well as documented tumor growth over time, also are risk factors for metastasis.
Small tumors generally are monitored for growth, using dilated fundus examinations, photography, and ultrasound. Sometimes laser photocoagulation or transpupillary thermotherapy (TTT) can be used to treat a small to medium tumor.
Medium to large tumors may be treated using a radioactive plaque (a small, gold-covered device containing a radioactive source). It even may be necessary to enucleate (remove) the eye completely, especially if tumor metastisis is suspected or confirmed.
Return to the Main Page 
of Anatomy, Physiology & Pathology of the Human Eye
 The color of the iris, established genetically, is determined by the amount of pigment present in the iris structure. No pigment at all (in the case of an albino) results in a pink iris. Some pigment causes the iris to appear blue. Increasing amounts of iris pigment produce green, hazel, and brown irises (or irides).
The color of the iris, established genetically, is determined by the amount of pigment present in the iris structure. No pigment at all (in the case of an albino) results in a pink iris. Some pigment causes the iris to appear blue. Increasing amounts of iris pigment produce green, hazel, and brown irises (or irides).